
Type 2 diabetes explained as simple as possible…
Type 2 diabetes is an elevation in blood sugars that occurs when a sugar called glucose can’t get into your fat and muscles where it is needed. Elevated blood glucose damages the lining of blood vessels, leading to a range of complications in the body's various organs.
Type 2 diabetes explained in a little more detail…
Type 2 diabetes is rapidly becoming the most common long-term disease in the world. More than 34 million Americans have diabetes (about 1 in 10), and approximately 90-95% of them have type 2 Diabetes. Type 2 Diabetes most often develops in people over age 45, but more and more children, teens, and young adults are also developing it.
The problem causing an elevation in the blood glucose levels occurs when there is a change in the insulin receptor's shape. In the normal situation, the body produces a small chemical called insulin (key) whose purpose is to bind to a receptor (lock) on the surface of fat and muscle cells, opening a channel to allow glucose to enter those cells. In type 2 diabetes, the shape of this receptor changes mostly due to weight gain around the stomach. The process of the lock changing shape is called Insulin Resistance.
What is metabolic syndrome?
Metabolic syndrome, sometimes called syndrome X, is a collection of disorders, including high blood pressure, insulin resistance, abnormal cholesterol levels, and excess fat around the waist. People with metabolic syndrome are twice as likely to have a heart attack and stroke and five times more likely to develop Type 2 Diabetes than people without metabolic syndrome.
Over the past three decades, the prevalence of Prediabetes (metabolic syndrome) has increased. More and more young people are showing signs of Prediabetes than ever before. The incidence of Prediabetes often parallels the incidence of Type 2 Diabetes and obesity. What’s scary is that a quarter of these adults don’t even realize that they have diabetes.
How common is type 2 diabetes?
The number of people diagnosed with diabetes is increasing; it’s estimated that:
- One in 10 people have diabetes (425 million)
- One in two adults with diabetes are undiagnosed (212 million)
- 12% of global health expenditure is spent on diabetes (USD $727 billion)
- Every 6 seconds, a person dies from diabetes
- Diabetes-related health expenditure will exceed USD $802 billion


Type 2 diabetes mellitus is a severe condition.
People with diabetes who have ongoing high blood glucose levels are at an increased risk of having poor health outcomes than people who do not have diabetes.
Statistics that relate to people with Type 2 Diabetes include:
- People with Type 2 Diabetes four times more likely to suffer heart attacks or strokes
- Type 2 Diabetes is the leading cause of vision-loss globally and is the fifth most common cause of preventable blindness and is the fifth most common cause of moderate to severe visual impairment
- Kidney failure is three times more common in people with Type 2 Diabetes.
- Amputations are 15 times more common in people with diabetes.
- More than 30 percent of people with Type 2 Diabetes experience depression, anxiety, and distress and have a higher alcoholism rate.
Early diagnosis, optimal treatment, and effective ongoing support and management reduce the risk of diabetes-related complications dramatically.
Who is at risk of developing type 2 diabetes?
There are several risk factors for Type 2 Diabetes. You are more likely to get Type 2 Diabetes if you are carrying weight around your belly. It is much more common in people from certain ethnic backgrounds like Indian, Middle Eastern, south-east Asian, and indigenous populations. In these groups, rates of Type 2 Diabetes are around 30% of the adult population. In Caucasian populations, the rates are more typically 10% of the adult population.

The risk factors which increase your chance of developing Type 2 Diabetes include:
- Have a family history of diabetes
- Being overweight, obese, or morbidly obese, particularly with extra weight around the waist
- Being physically inactive
- Eating a poor diet (one that is high in fat, salt, and sugar)
- High blood pressure
- Having signs associated with diabetes like skin tags and dark coloration around the neck and armpits called acanthosis nigricans
- Being older (over 55 years of age) – the risk increases as we age
- Over 45 years of age, being overweight, sedentary lifestyle, smoking or over drinking
- Ethnic background, including Pacific Islanders, Asian, and Southeast Asian, African Americans, Native Hawaiians, and Hispanics/ Latinos
What are the symptoms of type 2 diabetes?
The most common symptoms of Type 2 Diabetes Mellitus is not common at all. Part of the problem, the person, feels ok, but the damage is already occurring. Many people experience tiredness and fatigue, which is really noticed when you start to get sugars under more control. When the blood sugar levels are grossly elevated, people may notice excessive thirst and trips to the bathroom to pass urine. This occurs as high blood sugars pass into the urine and go into the water with the sugar.
The general symptoms and signs of type 2 diabetes include:
- Fatigue and irritability
- Excessive thirst, frequent urination, and dehydration
- Ongoing hunger
- Yeast and bacterial infections
- Dry and itchy skin
- Cuts and wounds that don’t heal quickly
- Pain and numbness in your feet or legs
- Blurred vision
- Changes in weight

Type 2 diabetes symptoms in MEN
Symptoms of Type 2 Diabetes Mellitus in MEN are often related to sexual health and function.
- Erectile dysfunction
- Retrograde ejaculation
- Urologic issues, including overactive bladder, urinary tract infections, and inability to control urination
- Decreased sex drive
Type 2 diabetes symptoms in WOMEN
Symptoms of Type 2 Diabetes in WOMEN also often relate to sexual health and function.
- Vaginal and oral yeast infections and vaginal thrush
- Urinary tract infections
- Female sexual dysfunction
- Polycystic ovary syndrome

How is type 2 diabetes diagnosed?
Most people diagnosed with Type 2 Diabetes are picked up by chance based on high blood glucose noticed in routine testing. This is not the best way to test for Type 2 Diabetes, and so more formal and targeted tests should be asked for. This is typically a glucose tolerance test or a Hb A1c test. A glucose tolerance test involved a fasting blood test, 75g of glucose as a sugary drink, followed by another blood sugar test taken 2 hours later. Diagnosing Type 2 Diabetes should not rely solely on using a Hb A1c test.
What is the Hb A1c test?
The Hb A1c test, or the glycated hemoglobin A1c test, is a blood test that can be taken at any time and is not affected by food. You don’t need to fast before taking the test. It indicates what your average blood glucose levels have been over the previous three months by measuring the percentage of a certain type of hemoglobin, called HbA1; a glucose molecule has altered that has attached to it. After glucose has been attached to hemoglobin A1 (HbA1), it is given a new name, Hemoglobin A1c or Hb A1c.
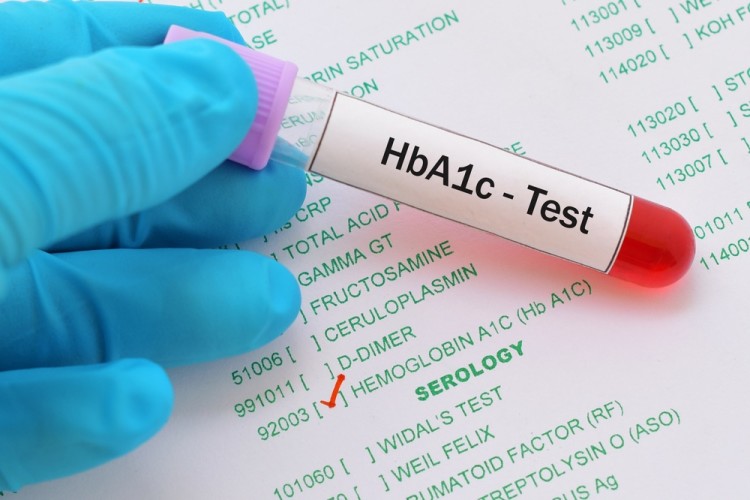
As mentioned, the Hb A1c test should not be used to diagnose Type 2 Diabetes. HbA1c can be a useful measure of blood glucose control, but it’s important to remember that it is only an indirect measure of blood glucose control. There may be other conditions for some people with diabetes that can cause a falsely low or falsely high Hb A1c reading.
Type 2 Diabetes Complications
Type 2 Diabetes is a vascular disease, which means it affects blood vessels. Complications in Type 2 Diabetes can be described as microvascular (small blood vessels) or macrovascular (large blood vessels) complications (Microvascular and Macrovascular Complications of Diabetes). Type 2 Diabetes-related complications occur over time due to persistent high blood glucose levels, high blood pressure, and abnormal cholesterol levels. These complications are serious and can be life-threatening.
Macrovascular complications – Problems with large blood vessels
Macrovascular affects the larger blood vessels in our body that supply blood to the heart, brain, and legs. Macrovascular complications include:
- Coronary artery disease can lead to a heart attack.
- Cerebrovascular disease can lead to a stroke.
- Peripheral artery disease can lead to pain deep in the leg muscles (calves, thigh, or buttocks) during activity and amputations.
Microvascular complications – problems with small blood vessels
Like macrovascular disease, ongoing high blood glucose levels are an important risk factor for developing microvascular disease in patients with type 2 diabetes. Microvascular complications include:
- Retinopathy – Disease of the eye which can lead to blindness
- Neuropathy – Disease of the nerves which can lead to foot ulcers requiring amputation
- Nephropathy – Disease of the kidneys which can lead to kidney failure and the need for dialysis
Hb A1c and complications in Type 2 Diabetes
Higher Hb A1c readings are also linked to an increased risk of complications.

How is type 2 diabetes treated?
Maintaining a healthy weight through a healthy diet and regular physical activity is not only important in your type 2 diabetes treatment, but it is important for your overall health and well-being.
Type 2 Healthy diet
Understanding what food you can eat and what quantities can be difficult, and there is no set Type 2 Diabetes diet. It can take some time adjusting to a diet change, even if they’re only small changes. A healthy diet for people with Type 2 Diabetes is very similar to a healthy diet of people without Type 2 Diabetes. The difference is that people with Type 2 Diabetes Mellitus need to be aware of their carbohydrate intake. Carbohydrate counting is a good option for people with Type 2 Diabetes because it can help space carbohydrate intake out across the day.
Adopting a healthy diet can also aid in weight loss.
Physical activity
Regular exercise has great benefits for everyone, including people with Type 2 Diabetes! Exercise has the ability to lower your blood glucose levels by moving glucose into your cells, where it’s used for energy. Exercising can increase your insulin sensitivity, meaning that your body needs less insulin to move glucose from the blood and into the cells.
When exercising, you should aim for at least 30 minutes or more of aerobic exercise on most days of the week and strength training (lifting weight, Crossfit, yoga). You could even break it up into three lots of 10 minutes and spread it across the day! Remember, if it has been a while since you were last active, start slowly and build gradually. We highly recommend you find an accountability partner.
We are here to help too! Learn more about our Reset Metabolic Weight Loss Program.

Monitoring blood glucose levels at home
Monitoring Type 2 Diabetes is important and includes blood glucose levels! You may be checking and monitoring your blood glucose levels around four times per day, or even more if you’re using insulin. Careful and regular daily monitoring is the only way to ensure that your blood glucose levels remain within the target range. If you have Type 2 Diabetes and you aren’t using insulin, you will likely check your blood glucose levels less frequently throughout the day. We have supplies and training at our clinic.
Regular blood tests with your doctor
In addition to daily monitoring, you should have a blood test every three months to check your Hb A1c. Hb A1c is a measure of your average blood glucose level over three months. Hb A1c test is a good indicator of how well your diabetes treatment plans have been going overall. Your target levels may differ from someone else due to your age or what medications you may be taking to help with your diabetes management. We have onsite blood testing available.
Oral or other medications
Sometimes oral medications are given to people with Type 2 Diabetes, for example, metformin. Some of these medications can stimulate your pancreas to produce and release more insulin. Other medications can inhibit the production and release of glucose from your liver, which means you need less insulin. One of the most common medications is metformin. This is typically the first medication prescribed to people with Type 2 Diabetes.
Medications used to treat type 2 diabetes include:
- Biguanides like Metformin
- Sulfonylureas such as Glimepiride, Gliclazide, and Glibenclamide
- SGLT2 inhibitors
- Thiazolidinediones (Glitazones) like Actos
- DPP4 inhibitors like sitagliptin, Vildagliptin, Saxagliptin, and linagliptin.
- GLP-1 analogs either daily or once weekly (such as Trulicity)
- Insulins with long-acting basal, mixed insulins such as Ryzodeg as well as a bolus or prandial insulins.
Insulin
People with Type 2 Diabetes or Gestational Diabetes use insulin too. Insulin is also necessary for people with type 1 diabetes.
There are many different types of insulin products available. This includes rapid-acting insulin, intermediate insulin, a mix of rapid and long-acting, and long-acting insulin. The type of insulin you use depends on your treatment plan. Diabetes Specialists may prescribe you a combination of insulin types to use throughout the day and night.
If you use insulin as part of your Type 2 Diabetes treatment, you need to keep in mind that where you store your insulin impacts the insulin’s effectiveness. Storing insulin in the fridge in an incorrect place can result in your blood glucose levels running higher than normal.
Is there a special diet I should follow if I have type 2 diabetes?
You may have heard of a ‘diabetes diet,’ but there is no specific diabetes-friendly diet! There are, however, certain foods that you should prioritize over others. A healthy diet focuses on a wide variety of fruits and vegetables, whole grains, lean proteins (i.e., red meat and fish), and low-fat dairy. These are foods that are packed with essential vitamins and minerals and lower in fat and energy.

Limiting the amount of saturated fats, refined carbohydrates (white bread and pasta), and sugary foods are also important. On the note of sugary foods, it is ok to have them sometimes, but they should be limited and treated as an occasional food item.
Carbohydrates and Type 2 Diabetes
You might have heard people talk about sugar and diabetes. Sugar is actually one form of carbohydrate! In addition to sugars, other forms of carbohydrates include starches and some types of dietary fiber.
Carbohydrates, or carbs, are important because they can significantly impact your blood glucose levels if you have Type 1 Diabetes, Type 2 Diabetes, or borderline Prediabetes. A perfect way to remember which foods contain carbohydrates is to think about foods that come from plants like fruit, seeds, and grains. The other major source of carbohydrates is dairy foods. Generally, dairy foods contain carbohydrates. There is carbohydrate in milk but very little to no carbs in cheese.
ReSet, our Metabolic Weight Loss program can help you with learning better eating habits.

Should I follow a low carb diet if I have Type 2 Diabetes?
People with Type 2 Diabetes may find a low carb diet useful in managing their weight, and this has shown to be effective and reasonably safe in short term trials. However, like in Type 1 Diabetes studies, there is limited evidence for long term weight management. Often, people find it difficult to stick to very low carb diets (ketogenic) and find a more moderate carbohydrate approach is easier (that is around 130g carb each day).
If you have Type 2 Diabetes, you don’t need to follow a low carb diet, but you need to be aware of the amounts of carbs you’re eating. There are some simple ways to reduce the number of carbs in your diet without losing flavor. One example is when making mashed potatoes, try combining a half mashed cauliflower with half mashed potatoes. 1 cup of potato/cauliflower mix is equal to 17g of carbohydrate compared to 1 cup mashed potato, which equals 30g of carbohydrate. This means that 1 cup of mashed potato on its own is equal to two portions of carbohydrate.
You can also learn more about dieting and carbohydrate counting by joining ReSet. Understanding how carbohydrates impact your blood glucose levels and how to count carbohydrates will make a huge impact on better managing your Type 2 Diabetes. By managing your condition well, you can reduce your risk of developing complications of Type 2 Diabetes.
What can I do to prevent type 2 diabetes?
There are changes you can make to improve your health and reduce your risk of developing diabetes. These include:
- Eating well
- Moving your body more daily
- Being and maintaining a healthy weight
- Setting realistic goals
- Getting support
- Make changes part of your everyday
There is also some evidence that suggests quitting smoking can help to reduce your risk of developing diabetes. Quitting smoking can help to lower your risk of having a stroke or heart attack as well.
Making these changes can also help to reduce your risk of developing diabetes comorbidities; hypertension and dyslipidemia
Can Type 2 Diabetes be reversed?
Ahh. What a great question. The honest answer is yes, Type 2 Diabetes mellitus can be reversed for some, but that is not true for everybody.
The sooner you start to treat and manage diabetes, the greater pancreatic function remains, the better your chances. Whether it is reversible or not doesn’t change that fact improving your diet and exercise and using the right medication all lead to dramatic improvements. Fundamentally, it is not diabetes that damages the body but high blood sugar. Most people manage their diabetes with the help of a medical team and use medication. Ask us about Metabolic Weight Loss, Gastric-Bypass, or Gastric-Sleeve surgery options.

What should I do next?
If you experience any Type 2 Diabetes symptoms or have Type 2 Diabetes risk factors, it is important to get tested as soon as possible. Some people are at higher risk and need regular testing.
If you are 45 years or older or have other risk factors for diabetes, you will require more frequent testing. By diagnosing and treating Type 2 Diabetes early, you decrease the risk of developing diabetes or delaying type 2 diabetes complications, for example, nerve damage, blindness, and heart disease.
It is important to know that diagnosing type 2 diabetes should not rely solely on using a Hb A1c test; call for an appointment NOW, and let’s work together to create a treatment plan just for you.

